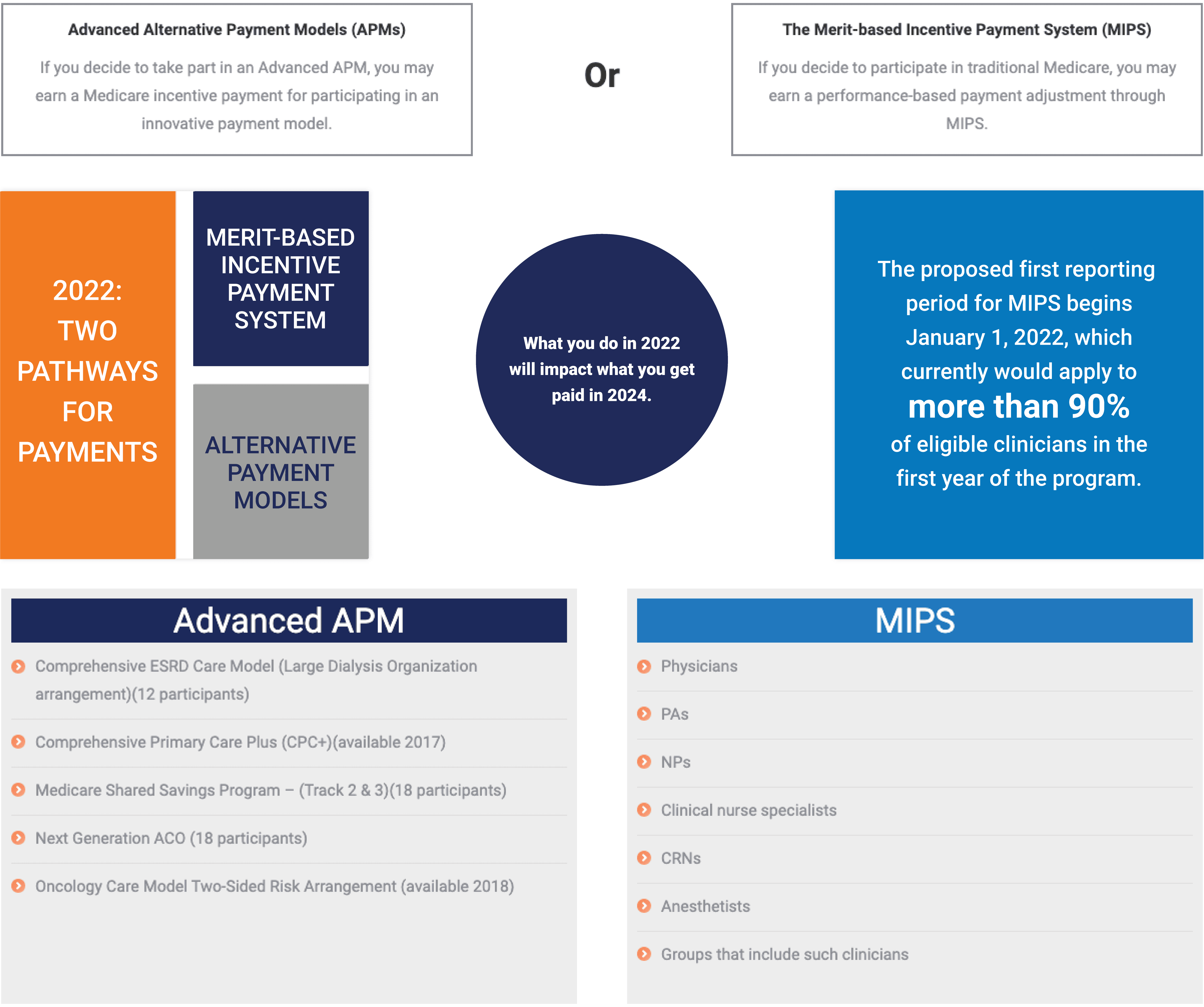
The Quality Payment Program as part of The Medicare Access and CHIP Reauthorization Act of 2015 (MACRA) is bipartisan federal legislation. MACRA repeals the Sustainable Growth Rate (SGR) Formula that has determined Medicare Part B reimbursement rates for physicians and replaces it with new ways of paying for care.
Under the Quality Payment Program, participating providers will be paid based on the quality and effectiveness of the care they provide. A large percentage of the physician payment will be based on value and outcomes of their care (not on volume). High value care commonly referred to as value-based care will be defined by measures of quality and efficiency and providers will be incentivized or decremented based on their performance against those measures.
CMS believes that the Quality Payment Program improves Medicare by helping you focus on care quality and the one thing that matters most — making patients healthier.